Pharma SFE Is Dead. Time to Move to a New Age SFA
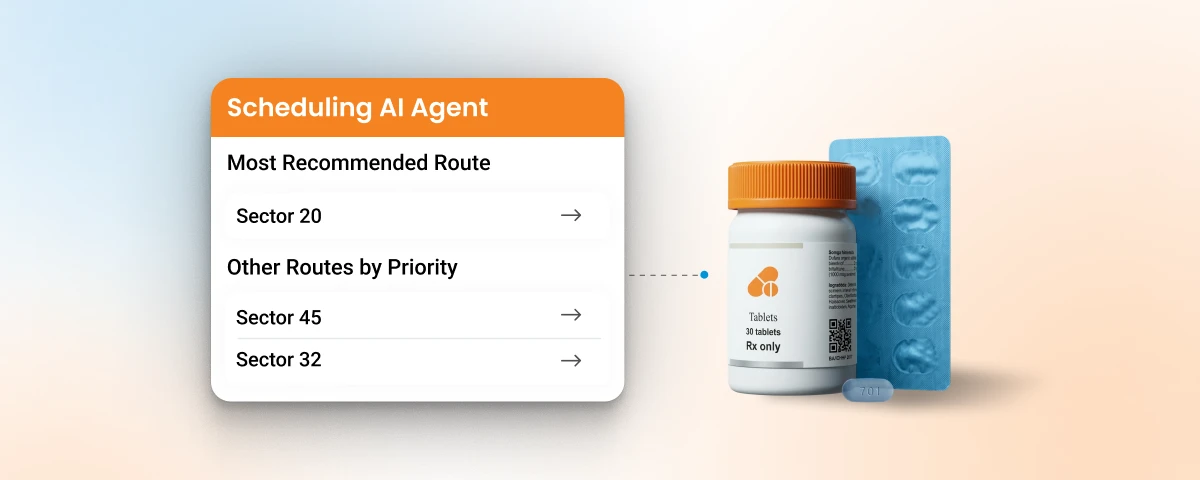
Table of Content
TL;DR Traditional pharma Sales Force Effectiveness programs track calls and visits but never measured prescription outcomes. This article covers why legacy SFE is failing and how BeatRoute’s Goal-Driven AI replaces it with outcome-linked field execution.
Pharma companies have spent decades on Sales Force Effectiveness programs: tracking calls, measuring adherence, counting doctor visits. The problem is that activity dashboards no longer move prescriptions. Prescriber behavior shifts, sample compliance gets audited, and institutional channels sit outside the SFE stack entirely, yet most tools still report on what reps did last week.
BeatRoute replaces legacy pharma SFE with Goal-Driven AI, automating call plans and linking detailing to field execution.
This is a walk-through of where traditional pharma SFE falls short and what an AI-driven pharma SFA actually changes, from prescriber scoring and sample tracking to journey plan validation and institutional rate contracts.
Why it matters
Traditional pharma SFE tools were built to answer one question: are reps doing what they’re supposed to do? That question is no longer enough. The companies pulling ahead are asking a harder one: are reps doing the right things? The gap between those two questions is where growth lives, and where traditional pharma SFE tools fall completely flat.
SFE measured activity. It never measured outcomes
The core promise of SFE was visibility. Are reps in the field? Are they meeting doctors? Are they submitting reports?
That was enough for a while.
The problem: Knowing a rep completed their calls today tells you nothing about whether those were the right calls. Knowing a doctor was visited three times this month tells you nothing about whether their prescribing behavior moved.
Traditional pharma SFE tools tracked activity. They never connected activity to outcomes. Pharma companies built entire field force structures on top of that without noticing the foundation was shaky.
The prescriber classification problem
Most pharma companies have a system for classifying doctors. Occasional prescriber. Regular prescriber. Prolific prescriber. The thresholds are defined by an internal matrix, how many prescriptions in a given period puts a doctor in each bracket.
It looks rigorous. It isn’t.
Why: The classification is entered manually by the reps or brand, for every brand they promoted, for every SKU they sampled. A rep promoting five brands to one doctor may need to enter prescriber status for five different brands, from their own judgment.
Two reps visiting the same doctor can classify them differently. The same doctor can be a prolific prescriber for one brand and an occasional prescriber for another, and that distinction matters enormously for targeting and sampling decisions.
Traditional pharma SFE tools capture the classification. They don’t validate it, trend it, or flag when it shifts.
A new age SFA Farmasi builds prescriber scoring from actual evidence, RCPA data, sampling history, POB trends, and surfaces the signal automatically. BeatRoute’s Customer Insights Agent does this at the visit level, giving reps prioritized tasks based on what the data says about each doctor, not what the rep remembers.
Sample management is a compliance problem hiding in plain sight
Pharma companies have strict sample rules. One SKU, one doctor, 45 units maximum in a year. Maximum 5 units per visit. GST applies. Documentation required.
Traditional pharma SFE tools don’t enforce any of this.
The bottom line: The rep is supposed to track their in-hand sample balance mentally, how many units they received for the quarter, how many they’ve distributed, how many remain. Every time they issue samples to a doctor, the running balance should update. It doesn’t, because the system doesn’t track it.
The compliance risk is real. The audit exposure is real. And it’s entirely a systems problem, not a people problem.
BeatRoute tracks in-hand sample balance in real time. The rep sees the available quantity against each SKU before the visit. The system counts down after every issuance. When the per-visit cap is hit, the system blocks the rep from entering a higher quantity. When the annual limit is approaching, the signal is visible. Compliance stops being the rep’s memory. It becomes the default.
Journey plans are locked. The market isn’t
Here’s how monthly planning works at most pharma companies. Reps build their monthly tour program on a mobile app. It goes to the area manager for approval. Once approved, it’s locked.
The area manager approves it by checking whether enough calls are planned, whether visit frequencies are met, whether important doctors are on the schedule.
The problem: That check happens once, at approval time. If a high-value doctor gets missed in week two, the area manager finds out at month end, not week two.
Pharma sales ops leaders describe exactly this gap: the area manager should be able to see during the approval itself which doctors from the master list are missing from the plan, which visit frequencies aren’t being met, which calls are below the daily average. Not as a report after the month ends. As a check before the plan is approved.
Traditional pharma SFE tools approve plans. They don’t validate them.
BeatRoute’s Scheduling AI Agent scores every doctor in the territory by priority based on visit frequency, recency, prescriber status, and coverage gaps, and surface deviations before they become missed opportunities. BeatRoute Kopilot proactively alerts area managers to inactive reps, overdue visits, and territory drift without waiting for a report request.
The area manager sees activity. Not the risk
Ask any pharma area manager what their dashboard shows. Call completion rates. TP vs actual. Report submission status.
What it doesn’t show: Which doctors in the territory have missed their visit frequency target. Which reps are behind on their sampling plan. Which high-value accounts haven’t been visited despite being on the beat plan.
Traditional pharma SFE tools show what happened. They don’t show what’s about to go wrong.
The area manager needs to see at approval time, not month end, how many doctors were missed, which ones were supposed to be visited twice but are only planned once, and where the daily call average is falling short.
BeatRoute Copilot gives area managers conversational access to exactly this data on their phone, without opening a dashboard, without waiting for an analyst to pull a report. The question gets asked. The answer comes back immediately.
The same rep does five different jobs. traditional pharma SFE tools handle one
In a single pharma field visit, the same rep might:
Detail a doctor and capture prescriber status per brand. Issue samples and track in-hand balance. Do an RCPA at the attached pharmacy, capturing which brand was prescribed, whether a competitor was substituted, the prescribing doctor’s name, the quantity. Book a personal order from the chemist if the doctor’s pharmacy is adjacent. Log whether any inputs were given.
All of this happens in one visit. Traditional pharma SFE tools break these into separate modules, or separate systems, or leave them uncaptured entirely.
The bottom line: When field activity is split across tools, the data is split too. Split data produces split insights. Split insights produce the wrong priorities.
BeatRoute runs every pharma field workflow, doctor visit, e-detailing, sampling, RCPA, POB, group meetings, on a single configurable app. One platform. One data layer. Every action in the same system, feeding the same intelligence engine.
Institutional sales has no home in traditional Pharma SFE tools
Government hospitals. Nursing homes. Private institutions. Rate contracts that run for months or years. Volume-based slab discounts. Any doctor anywhere in the country can buy at a given slab, depending on how many units they order.
The institutional channel runs on a completely different sales motion. The rep visits the purchase officer. Settles a rate. Gets it approved up the chain. Assigns a distributor. Tracks supply. Uploads PO copies and supply proofs against each contract. Calculates credit notes for the distributor at the end of the cycle.
Why it matters: None of this maps to a standard HCP visit workflow. Traditional pharma SFE tools don’t try. The institutional channel ends up managed through email, WhatsApp, and offline documents, with no system of record and no audit trail.
BeatRoute handles this through configurable workflow tiles. The same zero-code layer that builds doctor visit forms and sampling flows also builds institutional rate contract workflows. The IRC lifecycle, document uploads, slab-based discount tracking, and credit note calculation all live in the same platform as the field visit. Nothing gets managed outside the system.
The shift that’s already happening
The pharma companies moving fastest right now didn’t just replace a tool. They made a different decision about what their field technology is supposed to do.
Traditional pharma SFE tools answered: are reps compliant?
A new age SFA answers: are reps effective?
Compliance is a floor. Effectiveness is a ceiling. In a market where every competitor has a field force and doctor attention is finite, the ceiling is the only number that matters.
Goal-Driven AI guides every MR toward the specific call outcomes your brand goals require. BeatRoute replaces compliance tracking with performance intelligence, giving reps the right goals, giving managers the right alerts, and giving companies the data to act before the month is already lost.
Want to see BeatRoute’s pharma SFA in action? Minta demo.
Pertanyaan yang Sering Diajukan
What is the difference between pharma SFE and pharma SFA?
Pharma SFE tools focus on measuring rep activity and adherence to a pre-set plan. Pharma SFA, especially an AI-driven one, focuses on outcomes: prescriber behavior, sample compliance, call-plan quality, and institutional sales. SFA uses the same field data SFE captured but turns it into priorities and alerts instead of dashboards.
Why is manual prescriber classification a problem?
Because different reps judge the same doctor differently for different brands, and classifications rarely get updated as behavior shifts. That produces inconsistent targeting, uneven sampling, and wasted promotional investment. Evidence-based scoring using RCPA, sampling history, and POB data removes the guesswork and keeps prescriber tiers accurate over time.
How does AI improve journey plan quality for pharma reps?
An AI scheduling agent scores every doctor in the territory by visit frequency, recency, and prescriber status, then flags which doctors are missing from a proposed plan before the area manager approves it. This catches coverage gaps at week one instead of month end, when the cycle is already lost.
Can one SFA platform handle institutional and HCP sales?
Yes, if it is built on a configurable workflow layer. The same zero-code tiles that power doctor visits, sampling, and RCPA can also model rate contracts, PO uploads, slab-based discounts, and distributor credit notes. That keeps institutional sales inside the system of record instead of running on email and WhatsApp.
What signals should a pharma area manager see in real time?
Missed high-value doctors, reps behind on sampling, territories where call averages are falling, and visit frequency breaches against the master list. Those are leading indicators. Call completion rates and TP-versus-actual are lagging and tell the manager the problem only after it has already happened.


